Epidemiology
Etiology
Erythema multiforme is a type IV hypersensitivity reaction which can be triggered by the following.
- Infections (most common): herpes simplex virus (HSV) (50% of cases), Mycoplasma pneumoniae, and fungal infections
- Drugs: e.g., barbiturates, phenytoin, NSAIDs, beta-lactam antibiotics (e.g., penicillins), and sulfonamides
Pathophysiology
- Trigger Exposure: The process begins with exposure to a trigger (most often HSV).
- Viral DNA Transport: In herpes-associated EM, viral DNA fragments are transported to the skin by peripheral blood mononuclear cells.
- Keratinocyte Expression: HSV genes within these fragments are expressed by keratinocytes (skin cells).
- Immune Cell Recruitment: This expression attracts HSV-specific CD4+ T helper cells to the area.
- Inflammatory Cascade: The CD4+ cells react to the viral antigens, releasing interferon-gamma, which starts an inflammatory cascade. This immune response damages the skin cells, leading to the characteristic lesions.
Clinical features
- Rash
- Acute onset, with progression from erythematous macules to papules and vesicles to target lesions
- Target lesions
- Characteristic of EM, appear a few days after the onset of rash, may be absent in some patients
- Target lesions have 3 zones: an inner dark red/brown zone, surrounded by a pale zone, and an outer erythematous ring
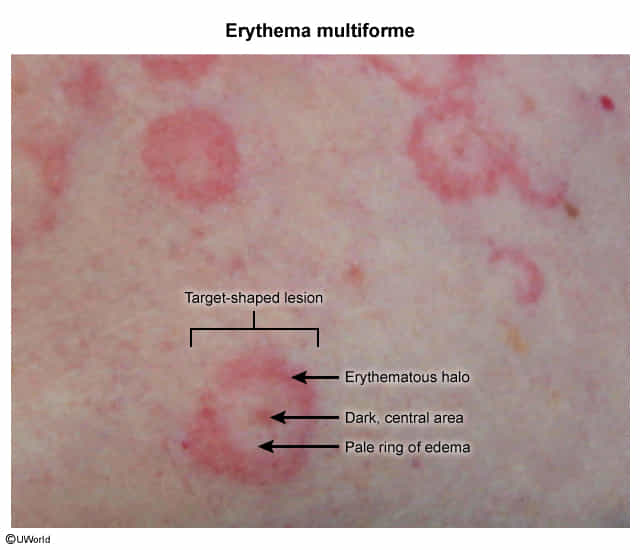
- Inner Dark Red/Brown Zone (Central Dusky Zone):
- This central zone represents the area of greatest epidermal damage.
- It is characterized by epidermal necrosis (cell death) of keratinocytes.
- There may be blister formation in this zone.
- Histologically, you might see vacuolization (formation of small cavities) in the basal cell layer of the epidermis.
- Pale Zone (Middle Edematous Zone):
- This zone surrounds the central dusky area.
- It is lighter in color and is characterized by edema in the dermis (the layer of skin below the epidermis).
- The edema is due to increased vascular permeability, which allows fluid to leak out of blood vessels into the surrounding tissue.
- Outer Erythematous Ring (Peripheral Red Ring):
- This is the outermost zone and has a red, inflamed appearance.
- This area involves:
- Perivascular mononuclear cell infiltrate: Immune cells (lymphocytes and monocytes) accumulate around blood vessels.
- Increased number of epidermal Langerhans cells (immune cells in the skin) and CD4+ T cell infiltration are observed.
- Expression of ICAM-1 and HLA-DR antigens on keratinocytes.
- The erythematous (red) color is because of vasodilation (widening of blood vessels) and increased blood flow in the area, which is a typical sign of inflammation.
- A study found that histamine metabolism can be impaired in the lesion. The activity of histamine-N-methyltransferase was significantly decreased in this area.